Understanding Coronary Artery Disease
Advanced technology is changing the typical process of cardiac testing and assessment so people experiencing chest pain can be informed of their health status quicker.
Chest pain makes 6.5 million people go to the hospital each year and it is the most noted symptom of a heart attack.2 Yet, luckily, most ER visits for chest pain are not life-threatening.
It is a diagnostic and logistical challenge for physicians to quickly tell the difference between people presenting with benign chest pain and those needing hospitalization and treatment.
Using advanced technology to illustrate artery disease that could be indicative of a heart attack, physicians can make this assessment in minutes. For you, this means less time waiting around for answers on heart health, less time spent in the hospital and less money spent on tests.
We think change is overdue
Peace of mind
Artrya Salix assists physicians in the rapid and convenient analysis of cardiac CT scans to screen for patients at risk of heart attack within minutes, whether in the emergency room or cardiologist’s office.
Within 15 minutes of the scan, patients with no concerning plaque buildup and, importantly, no underlying plaque features that pose a risk of heart attack, can return home, reserving diagnostic tests and hospital beds for patients who truly need them.


Let’s focus on what really matters
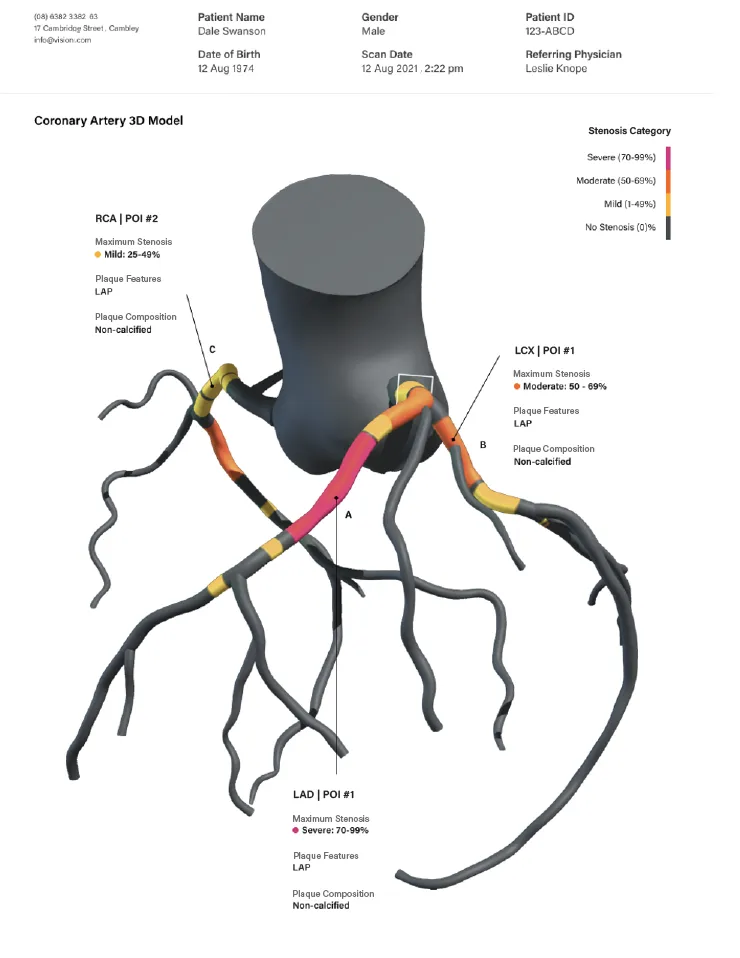
With advanced technology, physicians can visualize cardiac risk and create a tailored preventative therapy plan. This takes the guesswork out of trying to understand a complex and scary disease. Instead, this simple view of where disease is located and how much it has progressed within the artery, can help you share the decision-making with your physician on therapy, lifestyle and behavior adjustments required. Shared decision-making helps you take ownership of your future health.
Artrya provides tools to healthcare professionals only. Salix is used as an adjunctive tool and is not intended as a replacement for a health professional’s comprehensive review or their clinical judgment that considers other information from the CT images and the patient history.
References:
- Brown JC, Gerhardt TE, Kwon E. Risk Factors For Coronary Artery Disease. 2021 Jun 5. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan–. PMID: 32119297.
- Gulati M, Levy PD, Mukherjee D, Amsterdam E, Bhatt DL, Birtcher KK, Blankstein R, Boyd J, Bullock-Palmer RP, Conejo T, Diercks DB, Gentile F, Greenwood JP, Hess EP, Hollenberg SM, Jaber WA, Jneid H, Joglar JA, Morrow DA, O’Connor RE, Ross MA, Shaw LJ. 2021 AHA/ACC/ASE/CHEST/SAEM/SCCT/SCMR Guideline for the Evaluation and Diagnosis of Chest Pain: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2021;144(22):e368–e454. Study link. Published May 11, 2022.
